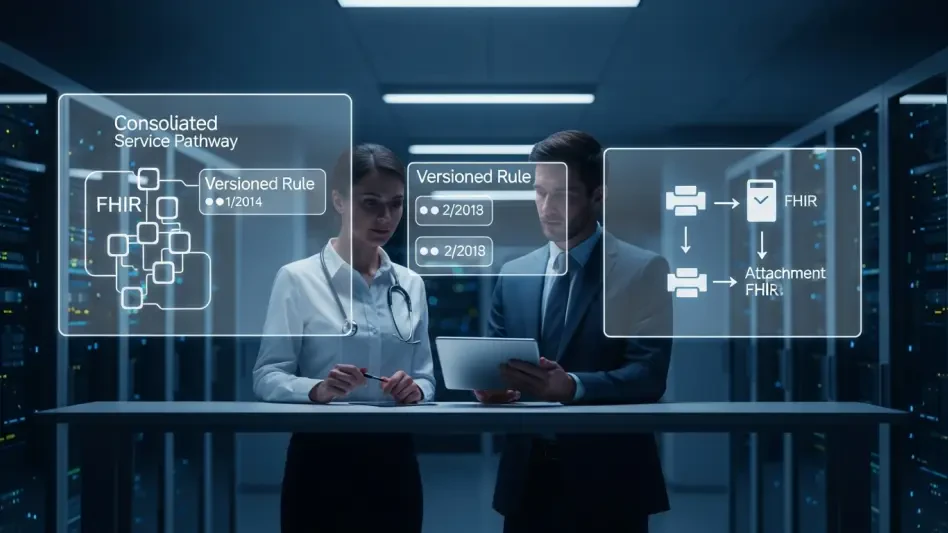
Prior authorization delays still drain clinician hours, derail care plans, and frustrate patients even as health plans roll out policy portals, FHIR APIs, and glossy dashboards that claim modernization, yet the promised speed rarely materializes because narrative rules do not compute themselves into decisions. This review examines whether the new wave of prior authorization automation—spurred by CMS-0057-F and built on FHIR pipes—actually converts interoperability into faster, fairer determinations, and what differentiates effective systems from cosmetic upgrades.
The core claim behind the technology is simple but disruptive: digitized policy is not automation. Converting policy PDFs into web pages and exposing endpoints makes information portable, but it does not resolve ambiguity, reconcile overlapping criteria, or execute logic. Automation that matters depends on turning medical-necessity criteria into machine-executable, clinician-aligned pathways with governance strong enough to withstand audits, appeals, and real-world complexity.
Foundations and Context: From Interoperability to Automation
Prior authorization sits inside utilization management, where the mandate is to ensure evidence-based care without stalling access. That tension is structural: guardrails must exist, yet guardrails cannot become roadblocks. Many organizations have chased speed by publishing policies and standing up FHIR endpoints, but most friction persists because reviewers still parse narrative text and free-form attachments by hand.
CMS-0057-F compels policy digitization and offers a transport layer for requests, responses, and attachments. However, interoperability is a highway, not a driver. Without computable logic, FHIR payloads shuttle unstructured stories back and forth, leaving determinations to human interpreters. The decisive upgrade is the shift from digitized narrative to executable policy: criteria that map to data elements, branch deterministically, and deliver explicit outcomes. The performance promise—lower burden, faster turnaround, consistent rigor—rests on that translation.
Core Building Blocks of Executable Policy Logic
Clinician-Aligned Decision Trees
High-functioning systems recast policy into stepwise, human-readable pathways that also compile cleanly into rules. Each node mirrors clinical reasoning—history, findings, differential, prior therapy, and objective measures—and ends with a single, defensible outcome. This is not an arcane ruleset; it is a clinical script rendered computable.
Determinism matters. Branches must be unambiguous, with stop/go criteria that eliminate the gray zones that fuel variability and appeals. The best implementations present just-in-time prompts, explaining why a question appears and what evidence satisfies it, so clinicians can traverse the path quickly while seeing the clinical logic behind the gate.
Separation of Clinical Criteria from Operational and Business Rules
A common failure mode is blending medical necessity with benefit design, network status, or site-of-service policies. That conflation yields inconsistent results and opaque denials. Mature platforms isolate clinical eligibility from operational checks, letting each layer evolve on its own cadence.
This design choice pays off operationally and legally. Clinical criteria can track guidelines and literature updates, while business rules reflect contracts and utilization levers. When a decision is contested, the system can show whether it hinged on medicine or on benefits, clarifying both remediation paths and accountability.
Consolidation at the Service/CPT Level
Providers often face a maze of overlapping policies tied to indications, modalities, and product lines. Consolidating them into one coherent pathway per service (for example, by CPT) slashes cognitive load and removes form roulette. The pathway can still branch by indication, but the entry point and outcome model stay consistent.
Consolidation also reduces maintenance overhead. Instead of amending five similar policies, authors update one pathway with shared subroutines. Over time, this drives consistency in evidence thresholds, reduces edge-case conflicts, and makes changes auditable and predictable for both plans and providers.
Sequencing and Data Capture Aligned to Clinical Workflow
Automation lives or dies on workflow fit. When questions follow the order clinicians document—history, exam, diagnostics, treatment, response—the system can pre-fill from the chart and only ask for gaps. Progressive disclosure keeps screens light, revealing additional criteria only when earlier answers require them.
Tight sequencing also improves data quality. If the system first confirms the diagnosis and phenotype, it can tailor subsequent prompts, avoiding irrelevant queries that erode trust. Mapping discrete EHR elements (ICD-10-CM, LOINC, SNOMED CT) to criteria reduces rekeying and speeds determinations without sacrificing specificity.
Governance, Versioning, and Evidence Traceability
Automation at scale amplifies both good and bad patterns. Robust governance prevents silent drift and ensures every decision is explainable. Leading platforms tag each rule with provenance—guidelines, peer-reviewed studies, consensus statements—and maintain versioned histories with clear effective dates and review triggers.
When evidence evolves or regulators ask for justification, auditors can see which version fired, why it fired, and how it maps to sources. This lineage is not bureaucratic overhead; it is the backbone of trust that lowers appeal rates and protects organizations when determinations are scrutinized.
Deterministic Engines and AI Assistants
Rules engines excel at executing stable logic and producing consistent outcomes; that reliability is the anchor of automation. AI augments the edges—extracting data from notes, mapping synonyms to standard codes, or suggesting likely next steps—without supplanting clinical judgment. The distinction keeps the system legible and auditable.
Meaningful metrics make the case. Accuracy is measured as concordance with clinician panels and retrospective gold standards; turnaround time captures both straight-through processing and escalations; auto-approval and appeal rates reveal whether speed compromises fairness. The best systems design for these metrics upfront, instrumenting every step so gaps become engineering backlogs, not guesswork.
Current Developments and Industry Momentum
The ecosystem is moving toward richer FHIR-based prior authorization endpoints, including structured attachments and document references that machines can parse. At the same time, computable guidelines libraries are maturing, giving policy authors reusable building blocks instead of starting from prose. These shifts enable automated intake and more precise evaluations.
There is also broader alignment on shared terminologies—ICD-10-CM, CPT, LOINC, SNOMED CT—and growing payer–provider workgroups that negotiate criteria in the open. The tangible change is a pivot from policy PDFs to governed artifacts that behave like software: versioned, testable, and deployable, with the audit trail regulators expect.
Deployment Scenarios and Real-World Use Cases
High-volume services such as imaging, labs, and DME benefit first because criteria are well-defined and documentation is structured. Straightforward cases flow through automatically, while exceptions escalate with context. Specialty therapies—oncology, rheumatology—see a hybrid model: deterministic gates on line-of-therapy and biomarkers, followed by targeted clinical review for nuance.
Embedding pre-service decision support inside ordering tools prevents avoidable denials by surfacing criteria while the order is being placed. Retrospectively, the same logic explains determinations during audits, tightening alignment between policy and evidence. Reported outcomes include days shaved from cycle times and measurable reductions in provider abrasion where pathways replaced narrative checklists.
Challenges, Risks, and How to Address Them
Ambiguous policy language, uneven data quality, and brittle cross-system mappings can undercut automation. The clinical risk is subtler: losing intent in translation or lagging behind new evidence. Operationally, change management remains hard; processes and incentives must shift alongside technology or the old manual work will simply reappear downstream.
Mitigations are well-understood but require discipline: standardized authoring playbooks, cross-functional governance councils, shared evidence libraries, and rigorous test harnesses that simulate real requests. Phased rollouts—starting with a narrow set of services and clear success metrics—build confidence while exposing edge cases early enough to fix them.
Outlook: Pathways to Scalable, Trustworthy Automation
What differentiates the leading approaches is not flashier AI but better policy engineering—authoring tools, lifecycle management, and explainability that clinicians recognize as sound. As structured clinical data and ambient documentation improve, more criteria can be pre-filled, turning prior authorization into a guided confirmation rather than a scavenger hunt.
Consensus pathways for common services are within reach as stakeholders converge on transparent criteria and share computable artifacts. If interoperability of clinical pathways and payer rules tightens further, real-time guidance could adapt to context while preserving determinism, creating a continuous learning loop that raises quality without adding burden.
Conclusions and Overall Assessment
The review found that interoperability laid the groundwork, but automation only delivered when policies were refactored into clinician-aligned decision trees with strict separation of clinical and operational rules. Systems that coupled deterministic execution with AI assistance, and backed both with governance and evidence traceability, achieved faster, more consistent outcomes and fewer appeals than rivals that relied on digitized narrative and manual review.
The verdict favored platforms that behave like regulated software: consolidated at the service level, sequenced to clinical workflow, and instrumented for accuracy, turnaround, and explainability. Next steps should prioritize policy refactoring, shared terminology mappings, and governance depth over additional endpoints or cosmetic AI. Done this way, prior authorization shifted from a bottleneck to an orderly checkpoint, accelerating routine care while reserving scarce human judgment for nuance where it mattered most.