Market Outlook: A One-Time Edit Reshapes the HAE Playbook
A single gene edit cutting hereditary angioedema attacks by 87% is forcing the HAE market to rethink risk, price, and care delivery all at once, and the clock on first-in-class approval has started. The headline efficacy for Intellia Therapeutics’ lonvoguran ziclumeran (lonvo-z) set off a strategic recalibration across payers, providers, and rivals, because a one-time in vivo CRISPR infusion would compete not only on clinical outcomes but on durability and total cost of care.
This analysis frames lonvo-z’s Phase 3 readout within the economics of HAE prophylaxis, weighs safety signals through a platform lens, and models how regulatory timing and outcomes-based contracts could shape adoption. The goal is to translate promising biology into market realities: who pays, who benefits, and how quickly practice patterns shift.
Moreover, the discussion connects clinical design to commercial traction. Washout of background prophylaxis before dosing strengthens the claim of independence from chronic therapy, while longer follow-up to week 104 becomes the fulcrum for launch positioning and pricing power.
Demand Drivers and Clinical Differentiation
HAE has long been managed with repeat dosing—monoclonal antibodies, kallikrein inhibitors, and bradykinin pathway blockers that suppress attacks but tie outcomes to adherence. These products anchored a sizeable specialty market by reducing ER visits and airway risk, yet they left a residual burden of injections, co-pays, and breakthrough events.
Genetic approaches shifted the curve. Antisense therapy such as Dawnzera pushed dosing to every four or eight weeks via autoinjector and set a high pricing watermark—about $57,462 per dose, or roughly $747,000 per year at four-week intervals. That benchmark sharpened payer scrutiny and, paradoxically, opened room for a steep but one-time alternative if it could credibly deliver multi-year relief.
Lonvo-z aims at the upstream driver: a liver-delivered CRISPR edit to permanently dial down a gene that fuels bradykinin production. In the randomized Phase 3, 80 participants were assigned to lonvo-z (n=52) or placebo (n=28) after washout. From weeks 5–28, attacks fell 87% versus placebo; 62% of treated patients were both attack-free and off prophylaxis, compared with 11% of controls. The magnitude and independence from background therapy underpin a differentiated value proposition.
Safety Profile and Platform Risk
Safety will decide the slope of adoption. Most adverse events in the HAE study—infusion reactions, headache, fatigue—were mild to moderate, and one transient liver enzyme elevation resolved within a week. On their face, these data suggest a manageable risk profile consistent with specialty infusion norms.
However, the market prices platform risk, not just product risk. Intellia’s separate in vivo program for transthyretin amyloidosis encountered grade 4 transaminase elevations and FDA clinical holds last year; those holds were lifted in March after agreement on enhanced liver monitoring and short-course steroid intervention. Investors now assume that similar safeguards will be embedded in lonvo-z’s label and REMS, tempering site activation speed but de-risking broader rollout.
The opportunity is a standardized playbook: front-loaded liver surveillance, clear steroid algorithms, and center credentialing that streamlines payer approvals. In contrast, reversible genetic suppression via antisense avoids permanent edits but requires lifelong dosing and sustained budgets—an important counterpoint for cautious clinicians and actuaries.
Regulatory Trajectory and Revenue Models
Intellia has begun a rolling FDA submission, with completion targeted for the back half of the year and a potential first-half 2027 launch. If approved, lonvo-z would be the first FDA-sanctioned in vivo CRISPR therapy, setting precedents on long-term follow-up, biodistribution reporting, and postmarketing commitments. Additional details are slated for the EAACI meeting in Istanbul this June, where durability and subgroup performance will face fresh scrutiny.
Commercially, the path runs through outcomes-based agreements. Payers are likely to peg milestones to attack-free durability at 12 and 24 months, steroid-sparing effects, and reductions in ER utilization. Amortized payment models or annuity structures could bridge budget impact, particularly if real-world data confirm sustained editing without late hepatotoxicity.
Pricing strategy will hinge on expected years of benefit. A premium over annual antisense costs could be justifiable if two to three years of attack-free status become the norm; anything less constrains the ceiling. Early adoption will cluster in specialized centers with integrated hepatology and pharmacy oversight, which can meet monitoring expectations and capture contracting value.
Competitive Dynamics and Market Share Scenarios
Current HAE incumbents retain strengths: known safety, self-administration, and established coverage pathways. Their defense will stress reversibility, familiarity, and predictable spend, while exploring label expansions and adherence programs to blunt switching.
Genetic competitors are unlikely to cede ground without price or convenience responses. Autoinjector-based regimens will emphasize at-home control and robust long-term safety records. Yet the psychological weight of “one-and-done” is hard to overstate; if yearlong freedom from attacks is reliably demonstrated, switching intent among high-burden patients should rise.
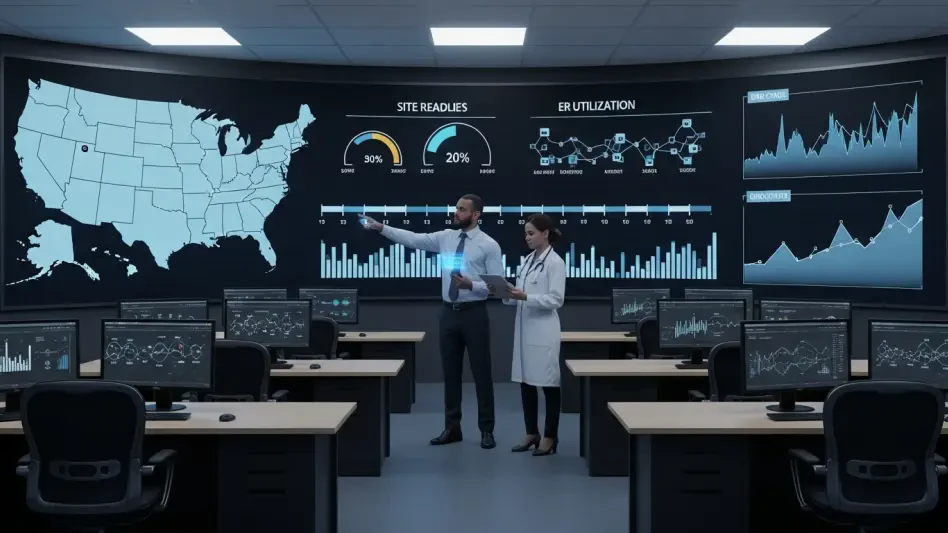
Base-case modeling suggests a gradual S-curve: limited initial throughput constrained by site readiness and monitoring protocols, followed by acceleration as real-world evidence validates durability. Upside scenarios rely on clean liver signals through year two; downside risks include heterogeneous responses across genotypes or late-emerging enzyme elevations that trigger tighter labeling.
Strategic Implications and Next Moves
For providers, readiness means building infusion pathways, codifying liver testing schedules, and training staff on steroid rescue algorithms. Systems that align immunology and hepatology under one roof will shorten time to therapy and enhance payer confidence.
For payers, piloting outcomes-based contracts tied to attack-free months and steroid-sparing metrics can hedge upfront exposure. Claims analytics should track avoided emergency visits and productivity gains to quantify value beyond drug spend.
For manufacturers and centers, patient education is pivotal. Clear explanations of permanence, monitoring expectations, and alternatives will enable informed consent and reduce churn from anxiety about editing. Data infrastructure that captures longitudinal outcomes will become currency in negotiations and a guardrail for safety.
Conclusion: From Signal to Standard
The market case for lonvo-z rested on three pillars: a striking 87% attack reduction versus placebo, an early safety profile that looked manageable with structured oversight, and a regulatory path that favored a first-in-class label with defined monitoring. Pricing power depended on durable attack-free intervals and streamlined delivery at specialized centers.
Payers and providers faced a practical trade: concentrated upfront cost versus multi-year relief from chronic dosing and acute events. The most credible route to broad access involved outcomes-based contracts and rigorous liver surveillance, turning platform caution into operational discipline. If durability held and safety stayed steady, adoption curves were set to steepen; if not, the therapy risked settling into a high-impact niche.