Introduction
The scientific landscape has shifted fundamentally for families grappling with the devastating realities of Leukocyte Adhesion Deficiency Type 1, a condition that once left pediatric patients virtually defenseless against the most common environmental pathogens. For decades, the medical community struggled to provide more than palliative care or high-risk interventions for those born with this ultra-rare genetic immunodeficiency. The recent regulatory emergence of Kresladi represents more than just a new pharmaceutical option; it signals a paradigm shift toward curative-intent gene therapies that address the root cause of systemic biological failures.
This exploration aims to clarify the mechanisms, clinical significance, and broader impact of this breakthrough treatment. Readers can expect to gain a comprehensive understanding of how the therapy works, its safety profile, and its role in stabilizing the future of rare disease research. By examining the transition from traditional stem cell transplants to personalized genetic engineering, this article provides a roadmap for understanding the current state of care for Leukocyte Adhesion Deficiency Type 1 in 2026.
Key Questions or Key Topics Section
What Is the Biological Basis for the Breakthrough of Kresladi?
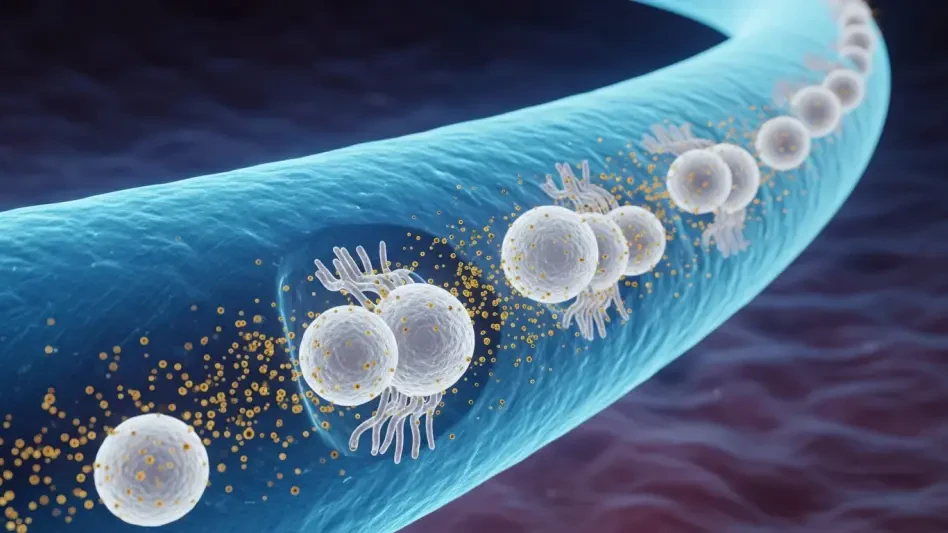
Leukocyte Adhesion Deficiency Type 1 is a harrowing diagnosis caused by specific mutations in the ITGB2 gene, which is responsible for producing the CD18 protein. This protein acts as a biological adhesive, allowing white blood cells to cling to the walls of blood vessels and migrate to the site of an infection. Without functional CD18, the immune system becomes an idle bystander; white blood cells remain trapped in the bloodstream, unable to reach tissues where bacteria or fungi are causing life-threatening damage. Historically, children with the severe form of this disease rarely survived infancy without an ideal bone marrow donor.
The innovation behind Kresladi, also known as marnetegragene autotemcel, lies in its ability to bypass the need for an external donor. It utilizes a lentiviral vector to insert a functional copy of the ITGB2 gene directly into the patient’s own hematopoietic stem cells. These cells are harvested from the patient, engineered in a specialized laboratory, and then infused back into the body. Once the modified cells engraft in the bone marrow, they begin producing a steady supply of white blood cells that express the necessary CD18 protein, effectively restoring the natural ability of the immune system to combat environmental threats.
How Does the Clinical Data Support Its Safety and Efficacy?
The transition from experimental concept to clinical reality was paved by robust data from Phase 1/2 trials involving pediatric participants. The primary concern for researchers was whether the newly introduced genes would remain stable and if the protein expression would reach levels sufficient to prevent infections. Clinical findings were remarkably positive, showing that 100% of the patients in the trial survived the follow-up period, a stark contrast to the historical mortality rates associated with severe LAD-I. This survival was accompanied by sustained CD18 expression, which remained consistent throughout at least two years of observation.
However, no advanced medical procedure is entirely without risk. Patients undergoing this treatment typically require a conditioning regimen to prepare the bone marrow for the new cells, which often results in temporary side effects like anemia and a reduction in overall white blood cell counts. Despite these manageable complications, the overall safety profile was viewed as highly favorable when weighed against the alternative of untreated disease or the risks of graft-versus-host disease associated with traditional transplants. The durability of the response suggests that a single infusion could provide a lifetime of immune protection.
What Does This Approval Mean for the Future of Rare Disease Medicine?
The regulatory path for this therapy was not without its hurdles, including a period in which manufacturing concerns necessitated a pause in the approval process. Nevertheless, the eventual accelerated approval by the FDA validated the underlying efficacy of the platform and demonstrated a willingness to prioritize life-saving innovations for ultra-rare conditions. As part of this process, the developer received a rare pediatric disease priority review voucher, a valuable asset that provides the financial flexibility to sustain research and development through 2027 and beyond.
Beyond the immediate benefits for LAD-I patients, the success of this treatment serves as a foundational milestone for other genetic therapies in development, such as those targeting Danon disease. By proving that a lentiviral-based approach can safely and effectively correct hematopoietic stem cells, the medical community has gained a vital template for addressing other inherited disorders. This progress ensures that the momentum in gene therapy remains strong, offering hope that the era of managing chronic illness is slowly giving way to an era of permanent genetic correction.
Summary or Recap
The clinical introduction of Kresladi transformed the management of Leukocyte Adhesion Deficiency Type 1 by providing the first-ever gene therapy for this specific immunodeficiency. By restoring the production of the CD18 protein through the modification of a patient’s own stem cells, the therapy achieved a perfect survival rate in its primary clinical trials. This success not only addressed a critical unmet medical need but also reinforced the financial and regulatory viability of the gene therapy sector. The ongoing collection of long-term data via post-marketing registries will continue to refine the understanding of its lifelong impact.
Conclusion or Final Thoughts
The achievement represented a major victory for patients who previously faced a future defined by isolation and frequent hospitalization. As the medical community observed the successful integration of genetic engineering into standard pediatric care, the focus shifted toward ensuring broader access to these specialized treatments. The journey of this therapy highlighted how rigorous scientific inquiry could eventually overcome even the most complex biological obstacles. It prompted many to reflect on how personalized medicine could soon become the standard of care for a wide array of previously untreatable genetic conditions.